The main goal of treatment is to interrupt the cycle of sphincter spasm and further tearing of the injured mucosa, thereby allowing the fissure to heal. This is carried out by advising the patient on the four pillars of treatment:
- Regulation of stool consistency
- Reduction of anal sphincter tone
- Relief of discomfort, bleeding and pain
- Allow healing of the fissure
These targets are achievable through a variety of measures that will be described.
Lifestyle Changes
Patients suffering from anal fissures should be encouraged to increase their intake of fluid and fibre. Stool softeners and sitz baths have virtually no side effects and often diminish the bleeding and pain. Additional comfort may be achieved with the use topical anaesthetics such as 2% lignocaine. Fluid intake should be adequate and a minimum of 8 to 10 glasses of water is recommended especially in our tropical climate. Simple hygiene practices such as the use of moist tissues or baby wipes is often a better alternative to toilet paper after bowel movements. If possible, using a shower spray for cleaning the perineum and padding dry is recommended.
Dietary advice includes increasing one's intake of fresh fruits, vegetables and bran cereal. Additional fibre supplements are also very useful in maintaining soft bowel movements.
Preparation of Sitz Baths
These warm baths provide soothing comfort to patients suffering from anal fissures by relaxing the anal tone and relieving the pain. They are prepared by adding lukewarm water to a shallow tub with or without an added 2 tablespoon of salt. A duration of 15-20 minutes is usually sufficient.
Healing rates of up to 50% can be expected with the institution of such measures.
Medication
The medical literature is filled with numerous studies addressing the efficacy of non-surgical treatments for anal fissures. It is therefore imperative that physicians be cognizant of the evidence that is available for each one of these. The following serves to summarise the treatment options the current available evidence on their efficacy.
The main intents of medical therapy are threefold:
- To promote internal anal sphincter relaxation
- To maintain the passage of soft stools in order to minimize further trauma to the mucosa around the fissure
- To provide pain relief
Topical Nitrates
These have been shown to improve the local blood flow and reduce the pressure exerted by the internal anal sphincter, thereby increasing the likelihood of healing. These are prepared in the form of a glyceryl trinitrate (GTN) paste or ointment at a 0.2% concentration. Most pharmacies are able to custom prepare these on request. Alternatively, commercially available preparations e.g. Rectogesic are available. Application around the perianal skin 2 to 3 times a day usually suffices. Patients must be warned of the reported 20-30% incidence of headaches as a side effect. These commonly occur about 30 minutes following application. In addition, patients on Sildanefil (Viagra) should avoid this form of treatment in view of the increased risk of hypotension. The comprehensive Cochrane review has found that the success rates of topical nitrates are only marginally better than placebo in the management of chronic anal fissures.
Topical Calcium Channel Blockers
These act mainly by reducing the internal anal sphincter pressure. Healing rates of 65-95% have been reported by several studies. Nifedipine and diltiazem (2%) are the 2 main topicals that have been studied. The advantages of these when compared to the topical nitrates are the lower incidences of headaches as a side effect. The efficacy of these agents has been shown to be equivalent to nitrates but there is currently insufficient data to conclude if they are superior to even placebo in healing fissures.
Botox for the other end
Injection of botulinum toxin into the internal anal sphincter results in what is commonly known as 'chemical sphincterotomy'. The resulting effect of a reduction of the internal anal sphincter pressure lasts for 2-3 months, allowing the fissure to heal. Patients are informed of the possibility of transient incontinence to flatus, which occurs in 10%. 5% of patients will experience incontinence to stools transiently. Failure rates of 20% have been reported.
This procedure is performed in the Colorectal Clinic under endoanal ultrasonographic guidance. Again, like the topicals, the data available does not show any significant advantage in efficacy when compared to the nitrates. However a single injection translates to convenience over the need for thrice daily topical applications of ointments.
Surgery
This is indicated when a trial of medical treatment has failed to produce any significant healing of the fissure, which is most commonly manifested as a persistence of pain. The goal of this is once again, to effect relaxation of the internal anal sphincter. This is achieved by an internal sphincterotomy, which essentially involves the surgical division of the internal anal sphincter from its distal most end to the level of the dentate line, or the most proximal limit of the fissure. The procedure is routinely performed as a day case, with the patient under either general or regional anaesthesia. It is performed through a small incision at the anodermal junction overlying the inter-sphincteric groove. This incision is placed laterally to avoid what is known as a keyhole deformity, hence the term ‘lateral internal sphincterotomy’.
The lateral internal sphincterotomy is the treatment of choice for anal fissures with success rates in excess of 90%. Symptom improvement is usually dramatic, and a median of 2-3 weeks is usually required for total resolution of symptoms. The major concern with the procedure is the risk of faecal incontinence. Although about 40% of patients will report some degree of incontinence in the first week, either to flatus or stools, studies have shown that only about 5% will suffer from mild incontinence to flatus 1 month post-operatively. Quality of life scores have been reported to be consistently good in patients following lateral internal sphincterotomy.
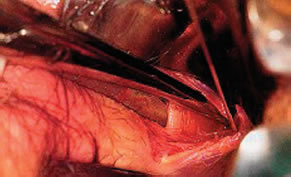
Sphincterectomy
Nevertheless, in view of these risks, patients who have had a history of anorectal surgery and multiparous women should only be offered lateral internal sphincterotomy with caution.